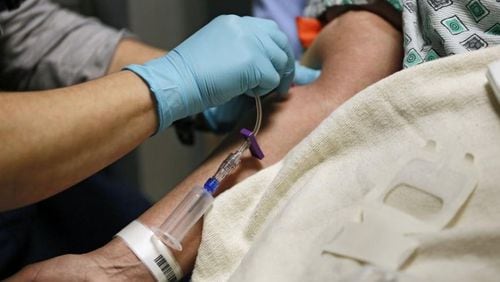
The nurse was seen on duty at the hospital with red, dilated eyes, her speech slurred, her behavior drowsy. Trusted to care for people at their most vulnerable and fragile, instead she had taken opioids intended for patients and injected herself.
Without a doctor’s OK, another nurse ordered Demerol and Benadryl for an emergency room patient, but that patient had already been discharged. Later, he found work in the hospital at Georgia State Prison, where he pilfered those same drugs and worked while he was impaired.
Yet another nurse went to work at a hospital so intoxicated she couldn’t operate a computer or an elevator, then she gave a patient the wrong medication.
All three are still on the job. So are most Georgia nurses ensnared in the opioid epidemic, even those who showed up at work stumbling, tampered with syringes to get a fix, or falsified patient records to cover up their addiction.
But the public can't know who all the addicted nurses are, what they did, or the extent of what some call a crisis, because of the way the state's regulatory board for nurses is operating, an Atlanta Journal-Constitution investigation found.
The Board of Nursing handles more than half of its disciplinary cases secretly, and it doesn’t keep statistics that would show how many nurses are addicted or how many relapse.
So when a registered nurse from LaGrange displayed “strange behavior” at work — and her supervisors found patients hadn’t received their medications 27 times — the board issued a confidential order. It came to light only after the opioid-addicted nurse failed to comply and had her license suspended.
Other nurses have been granted second, third and even fourth chances when they relapsed, the AJC found.
The board put a Forsyth nurse on probation in 2002 for chemical dependence, again in 2013 after she was fired for diverting morphine, and again in 2017, after yet another relapse.
The secrecy and leniency can put the public at risk.
Families hiring home-based nurses for elderly parents may have no way of knowing if they’re bringing in someone with a history of pocketing medications. Hospitals and nursing homes can hire a nurse having no clue about a prior history of drug abuse.
Rep. Sharon Cooper, R-Marietta, said the nursing board — all but one of whose 13 members are nurses — seems more concerned with protecting the profession than patients.
"We have boards to protect the public, not to be soft touches," said Cooper, chairwoman of the House Health and Human Services committee and herself a registered nurse. "I know how bad the drug problem is. And so I really think that the first priority should be to the patient's protection."
Janice Izlar, president of the nursing board since July 2016, says that is the priority. But secrecy, she said, helps get nurses more quickly under the board’s supervision, so they can be monitored and held accountable.
If the board goes to war trying to revoke licenses, Izlar said, it can spend months or years locked in legal battles; meanwhile the nurses would still be seeing patients without any monitoring. The lengthy investigative process, she said, often culminates with an addiction specialist certifying that a nurse in recovery is safe to practice, under conditions aimed at keeping them under a more watchful eye.
Instead, the board in many circumstances offers private orders as a negotiating tactic.
“Many times, the nurse does not want their name on a public Board of Nursing website that there has been discipline action,” Izlar said. “And so they will accept the order and actually get under monitoring and under appropriate care that has been determined by their physician.
“And they will actually sign this order much quicker, and they will go ahead and get into the programs and into monitoring much quicker.”
An addicted nurse must enter aftercare treatment, submit to random drug screens, notify employers, submit quarterly reports from employers and the nurse’s doctor, and stay out of jobs with access to drugs, among other requirements.
Hidden orders, hidden risks
Those terms end once the order ends, though. So the drug history of nurses who received private orders is concealed.
Patient advocates are alarmed at the high proportion of cases that the board keeps hidden.
Of 333 disciplinary orders the board issued in 2017, 54 percent were private, according to statistics the AJC obtained through an open records request. In 2016, 59 percent of 356 orders were private. Izlar said just under half of last year’s private orders were alcohol- or drug-related. She could not say how many involved opioids.
"We encourage consumers to do their homework about their hospitals and providers," said Beth Stephens, a senior policy director for Georgia Watch. "So if information about provider discipline is shielded from the public, it makes doing that research very difficult."
Sherry Sims, a retired nurse who volunteers to help recovering addicts through the Georgia Nurses Association’s Peer Assistance Program, said opioid abuse among nurses has reached a crisis level. On top of their easy access to prescription drugs and job stresses, nurses are especially at risk of addiction because their care-giving personalities make them less likely to seek help for themselves, Sims said.
Rep. Cooper said she doesn’t buy the argument that private orders get nurses into treatment faster. The board could also protect the public by exercising its powers of summary license suspension, she said. Georgia law says that when public health, safety or welfare “imperatively requires emergency action,” the board can quickly suspend a nurse’s license.
“I’m sorry if some nurse gets her license suspended, and that’s her livelihood,” Cooper said. “But if she’s in the position of putting patients at risk, then so be it.”
However, Izlar said that the state Attorney General’s Office has advised the board that it can’t issue an emergency suspension unless the threat to the public is imminent. By the time a complaint reaches the board, the accused nurse has usually entered rehab and been deemed safe.
Addiction experts say nurses in recovery should be allowed to work, without their names being divulged, so long as patient safeguards are in place and cases are handled consistently.
The Georgia board, though, can take months or years to act. And it's unclear why some addicted nurses get private orders and some don't. In the past 18 months, at least 65 nurses were publicly sanctioned for opioids, according to an AJC analysis.
Izlar says that nurses who have diverted drugs at work or worked while impaired can’t get private orders. When it comes to impairment issues, only nurses who self-report alcohol, marijuana or opioid abuse can get them.
With investigative records and private orders locked down, there is no way to verify if the board adheres to that unwritten policy. But the opioid-addicted LaGrange nurse got her private order in 2015, despite her “strange behavior” and medication discrepancies at work.
And some first offenders who self-reported got public orders.
Izlar said she can’t discuss specific cases. “Every case has its unique twists and turns,” she said.
Because of the inconsistency, and because most nurses who were publicly disciplined are in recovery, the AJC is not identifying the nurses who received public orders. Their orders are on the Secretary of State's website.
In the throes of addiction
One sanctioned nurse from Milledgeville said no one with the state ever gave her the option of keeping her drug addiction a secret, even though she self-reported and had only been in trouble once.
Much as she would have preferred a private order, she said she’s now opposed to the idea.
"As one who can attest to just how evil, manipulative, destructive addiction is, I hate to say it, but I probably have to come down on the side of being public with it," she said. "Because I know from personal experiences just how sick someone is when they're in the throes of addiction. The capacity to lie and manipulate is great."
“I knew how to manipulate the system to obtain more opioids,” said the nurse, who came off probation in November. “I basically broke the law to get them. It was a form of insanity.”
However, she spoke only on the condition that her name not be used since she is a recovering addict.
She got hooked the way that many people do: though a doctor’s prescription.
For her, it was a Lortab prescription for menstrual cramps. She found the drug not only erased her physical pain, but also the pain of depression she’d been battling most of her life. Within months, she was calling in prescriptions for herself, using a doctor’s DEA number.
“It was my choice to deliberately misuse that type of medication once I discovered that it made me feel better in more ways than one,” the 48-year-old said.
By 2012, she’d lost 40 pounds and got high after almost every work shift. Then on her way home from a Walmart run, she nodded off behind the wheel, crashed into a mailbox and got arrested for DUI.
It took about a year for the board to place her license on probation. Meanwhile, she entered the Peer Assistance Program, went to AA meetings and continued working as a nurse practitioner.
She’s since earned a post-master’s certificate in psychiatric mental health and is about to start a job with the Department of Veterans Affairs. She credits the nursing board and Peer Assistance with saving her life.
"I simply was bullheaded about not losing my nursing license, so that's what made me enter recovery and kept me there during the difficult time," she said. "Over time, as my brain healed, I started to think more sanely, and realized I certainly do not want to have the life of an addict."
Discipline or accommodation?
The AJC’s review of public orders found that when addicts land before the Board of Nursing, they usually avoid the heavy hammer of discipline, instead finding mercy. Some examples found in public orders available on the Secretary of State’s website:
- A McDonough nurse once bolted from a hospital rather than take a urine drug screen. For years, she bounced from hospital to hospital as a drug addict, showing up for work with dilated eyes and slurred speech and stealing Demerol. At an Athens hospital, she was absent from her station for long periods and left behind a syringe and needle in a bathroom. In 2011, she pleaded guilty to a drug offense in Monroe County and received court-ordered probation. The nursing board suspended her license in 2014 but gave it back this year after she provided evidence of treatment and 13 months of negative drug screens.
- In 2016, an Augusta nurse got fired from one job for diverting narcotics, then confronted by a hospital for stealing drugs, then convicted of a felony and put on court-ordered probation for taking Dilaudid from yet another hospital. Though she admitted to taking medications from patients, and though she failed to report the conviction to the nursing board within the required 10 days, the board put her license on probation so she could work after serving a three-month suspension.
- In 2011, a Jefferson nurse went into treatment for opiate dependency after stealing Versed, Fentanyl, Demerol and morphine from his employer for personal use. The board put his license on probation for three years. One month after his probation ended, he diverted morphine again. The board gave him five years' probation.
- In 2016, the Georgia Drugs and Narcotics Agency caught a Columbus nurse using doctors' DEA numbers to write illegal prescriptions. She admitted to engaging in the practice for "a long time." The nursing board gave her a reprimand, a $500 fine and an order to take online classes in ethics, accountability and prescribing.