Georgia patients still at risk from hospital-acquired infections
Years after public health officials declared war on hospital-acquired infections, Georgia still lags behind other states at protecting patients from dangerous conditions they can develop while being treated for something else.
When it comes to life-threatening bloodstream infections that come from central lines inserted into a large vein for care, Georgia ranks among the worst in the nation, according to an Atlanta Journal-Constitution review of federal data.
While some Georgia hospitals have made remarkable improvements, the state as a whole also ranks in the bottom half of states at shielding patients from urinary tract infections associated with catheters and from hospital-onset cases of MRSA — methicillin-resistant Staphylococcus aureus —a type of bacteria that does not respond to many antibiotics, the AJC found.
“These are terrible infections — it’s not like a cut to your finger that gets infected,” said Helen Haskell, a South Carolina-based patient safety advocate who is the president of Mothers Against Medical Error. “Even people who are very strong have aftereffects for years.”
Haskell said she hears the stories all the time of people entering the hospital for one thing and then get even sicker during their stay. “It’s part of the cascade,” Haskell said. “Somebody has an accident or an elderly person falls and they’re in the hospital for that, and they get all of these other infections.”
On a typical day, 1 in 25 hospital patients had at least one infection they got while in treatment, according to Centers for Disease Control and Prevention. In 2011, there were 722,000 infections resulting from health care. About 75,000 patients with these infections died during their hospitalization, according to research published in 2014.
This death toll and the giant costs of treating infections prompted public health officials and patient advocates to push hospitals to do better — and many hospitals across the country have made remarkable progress.
“I feel like we have a come a very long way, but we still have a long way to go,” said Lisa McGiffert, project director of the Safe Patient Project at Consumers Union. “The number of people who get infected every year, it’s still way too high.”
Strong, weak performers
Researchers have proven that many of the infections patients get while in treatment are preventable. But that requires close adherence to proven protocols — everything from rigorous hand cleaning and quick removal of catheters to set protocols for inserting central lines.
Some hospitals in Georgia have dedicated themselves to doing better and now stand out as some of the best in the nation. But others are rated as performing below national benchmarks and play a part in pushing the state toward the bottom of the rankings on some key infection-prevention categories.
In Georgia, for example, Emory University Hospital and Piedmont Atlanta Hospital are rated in the federal data as performing worse than the national benchmarks for controlling bloodstream infections associated with central lines. Meanwhile, WellStar Kennestone, Northside Hospital and Northeast Georgia Medical Center perform better than the national benchmarks, the AJC found.
Up to one in four of the patients who get these types of bloodstream infections may die, according to the CDC.
The newly released statistics reviewed by the AJC cover a hospital’s performance from April 1, 2016 to March 31, 2017. The infection data is collected through a CDC program and adjusted, based on the type of hospital and the patients it sees, in order to allow for fair comparisons.
The Georgia Hospital Association said 93 hospitals across the state have joined a partnership to improve patient safety. Between October 2016 and September 2017, GHA said, those hospitals improved central line-associated bloodstream infections by 33 percent. During the same period, those hospitals improved catheter-associated urinary tract infections by 16 percent, GHA said.
“We must remember that every hospital in every state is committed to that same goal of patient safety,” GHA said in a statement. “Therefore, a national ranking is not reflective of the improvements Georgia is making, because all other states are making similar improvements.”
The Georgia Department of Public Health will partner with GHA to work on the central line-associated bloodstream infections and catheter-associated urinary tract infections to try to lower Georgia’s overall rate, said Nancy Nydam, a department spokeswoman.
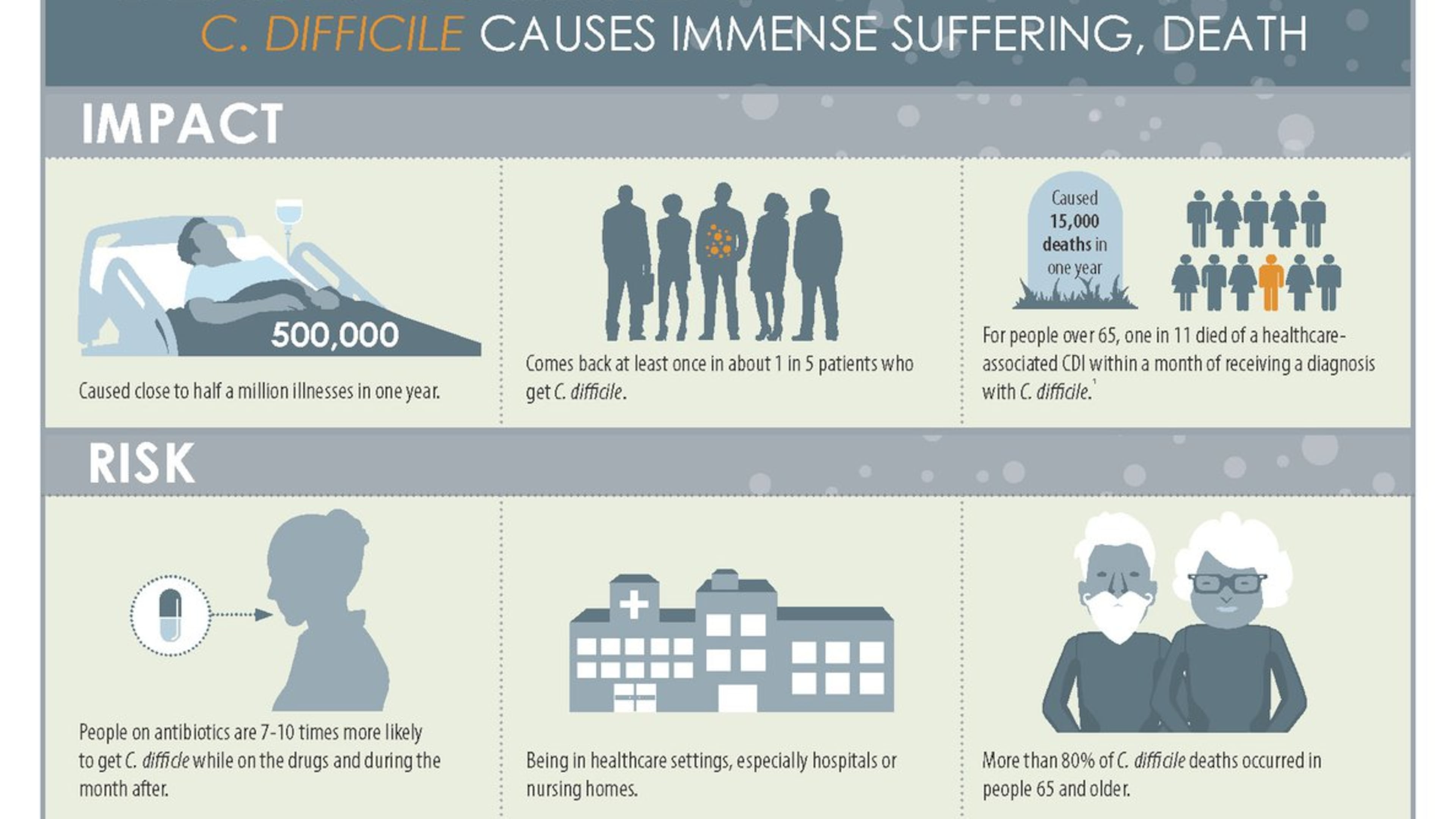
Georgia hospitals have been effective at reducing Clostridium difficile infections, Nydam said. Widely known as "C. diff," the infections cause inflammation of the colon and potentially-deadly diarrhea. Combating C. diff demands more astute prescribing of antibiotics, as well as religious handwashing in health care settings.
The federal data reviewed by the AJC show that this is a bright spot, with Georgia hospitals performing better than most states. Clostridium difficile caused about half a million infections nationwide in 2011, according to the CDC, and 29,000 people died within 30 days of being diagnosed.
Among 27 Georgia hospitals that stood out for strong scores on C. diff prevention were Grady Memorial, Piedmont Atlanta and WellStar Atlanta.
Frontline solution
For years, patients in Georgia had no idea how well their own hospital performed on infection prevention. Some states required public reporting. Georgia never did. But a federal program designed to drive down infection rates made public disclosure part of its strategy, and that has nudged many hospitals to do more to protect patients.
"Georgia was late to the game in public reporting and they've got some catching up to do," Haskell said. "There's nothing like a little sunshine to help people improve."
Medicare also tied payments to hospital performance, which added another carrot for hospitals to improve. It’s not an easy task to eliminate such infections. Busy doctors and nurses are often the vehicles whose hands carry germs from one patient to the next. Or, germs can live on surfaces in hospitals rooms that may appear to be clean but aren’t.
Every member of the hospital staff, from doctors on down, have to get it right with every patient every time to keep patients safe.
The WellStar Health System has a strong record for infection prevention. But the system has grown and added new hospitals in recent years. WellStar implemented a standardized system designed to make everyone involved in patient care an integral player in an infection-prevention program, said Dr. John Brennan, WellStar’s chief clinical integration officer.
The system successfully attacked C. diff rates, Brennan said, by getting pharmacists and doctors involved in wiser use of of antibiotics, and then it brought in hospital staff to nail down the best ways to perfect hand hygiene and isolation of any patients who come in with C. diff so it isn’t spread to others. He said the system used the same approach to combat other types of infections, which led to improvements that could be sustained over the long haul. Part of the approach is empowering all staff members to speak up, if they see something that could put patients at risk.
“This wasn’t about a top, high executive saying, ‘Do this and do that.’ This was about looking at the data, understanding the problem and having the frontline people help solve it,” Brennan said.
Once those protocols are set, they have to be hardwired into a system that uses safety checklists, just like pilots do before takeoff. “That checklist is done the exact same way, every single time and that’s the way that we’re looking at this,” Brennan said.
No excuses
When hospitals really devote themselves to preventing infections, they often see remarkable results.
Piedmont Healthcare set a goal of reducing the top-five hospital-acquired infections by 50 percent over three years.
During the fiscal year that ended in June, Piedmont already reached a 40 percent reduction. In the past six months, it registered another 20 percent drop.
Piedmont said its success relied on a “Promise Package.” That’s a tool that integrates everything from complex information and training on infections, to the detailed responsibilities and work flows of everyone involved in protecting patients.
It tracks performance, too.
With such results possible, it’s hard to tell patients that their infections simply couldn’t be avoided.
“Our goal is to eliminate preventable infections,” said Dr. James Steinberg, a professor of medicine in the division of Infectious Diseases at Emory University and chief medical officer at Emory University Hospital Midtown.
Steinberg said Emory’s hospitals had a 22 percent reduction in all healthcare-associated infections in the most recent fiscal year, which ended in June.
While Emory University Hospital was rated as performing worse than national benchmarks in some categories, Steinberg said the adjustments made in the federal data might not fully capture the complexity of the patients seen at a large teaching hospital like Emory. Indeed, some other highly-regarded teaching hospitals, including Duke University Hospital, also earn scores that are worse than national benchmarks in some of the federal infection-prevention categories, the AJC found.
Emory has implemented processes to make sure a patient is protected at key moments, such as when a central line is inserted.
But Steinberg said hospitals have to constantly monitor their data and processes.
Even turnover in staff can hurt any hospital’s efforts. “You think you have something conquered, and you think you have your processes perfect and reliable and hard-wired, and there is turnover and you may to revisit how you do things,” he said.
Hospitals across the country are working to implement the processes that make sure no step is forgotten.
“The span of work that needs to be done to make sure that every patient is getting the closest thing possible to perfect care, every single time, is a huge order,” said Dr. Michael Bell, deputy director of CDC′s Division of Healthcare Quality Promotion. “Setting up systems that will do that for us is part of the job at this point.”
Those in the patient safety movement say hospitals must commit to infecting none of the those who comes into their doors looking for a healing touch. That applies, they say, whether it's a perfectly healthy patient there for a joint replacement surgery or a seriously ill patient for whom an infection is likely to be deadly.
Some hospitals and some states have that mindset, McGiffert said. Others aren’t quite there yet.
“I do not think there is any excuse,” she said. “Hospitals should be moving closer to zero.”
By the Numbers
1 in 25
Number of hospitalized patients with at least one infection acquired while receiving medical treatment
722,000
Number of healthcare-associated infections in U.S. hospitals in 2011.
75,000
Patients with healthcare-associated infections who died during their hospitalizations.
Source: Centers for Disease Control and Prevention
Check out infection rates and other quality of care statistics for metro Atlanta hospitals at the AJC’s special Hospital Checkup site: hospitals.myajc.com



