As pandemic restricts hospital visits, many face illness alone

The urgent call, from an emergency room doctor at Emory Decatur Hospital, came on a Sunday morning. AnnaLisa Silliman-Patterson’s ex-husband, Matt Lindsey, had been admitted to the hospital and was very sick with COVID-19. Maybe the sickest the doctor had ever seen.
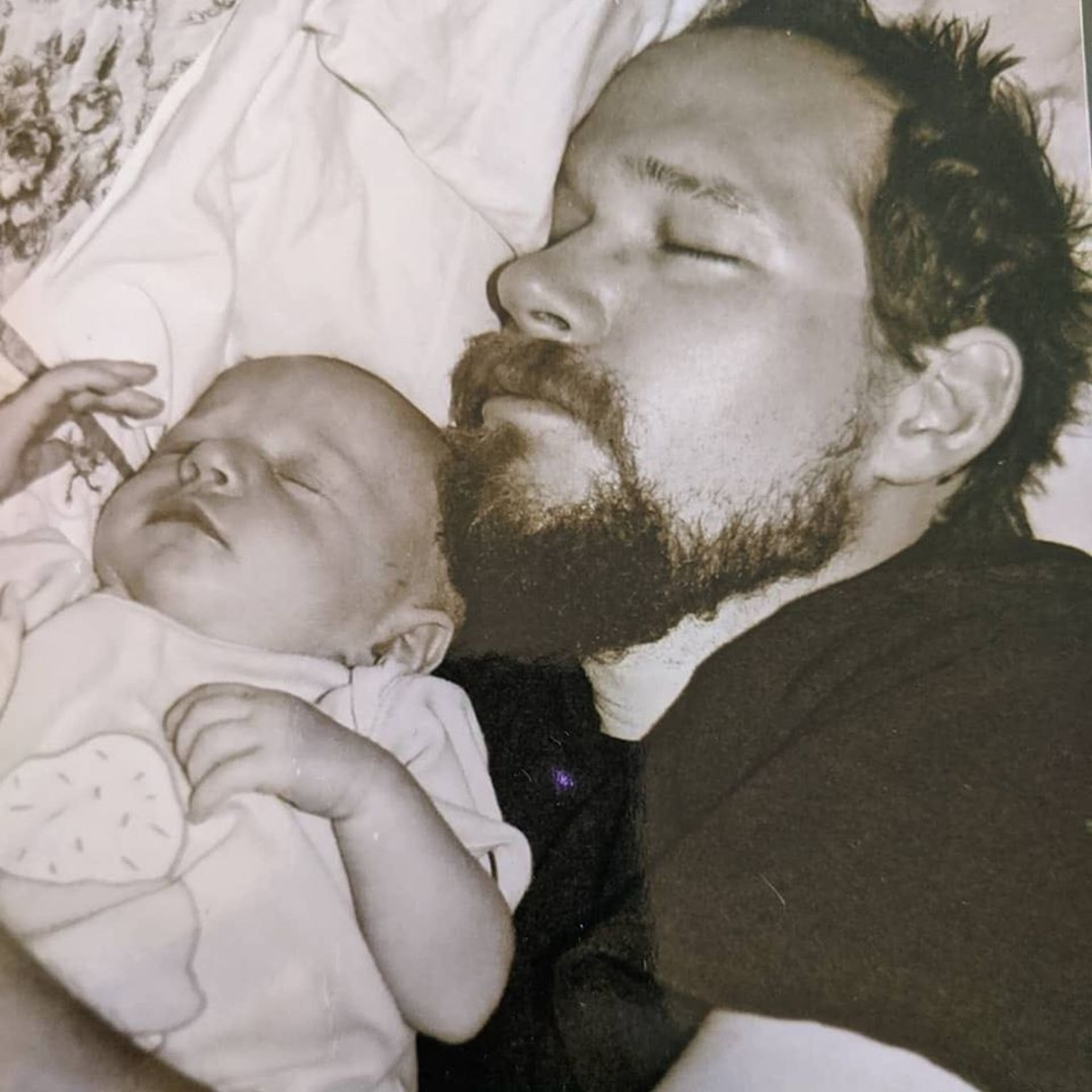
Lindsey — a 48-year-old doting father of three grown sons and a 15-year-old daughter — had driven himself to the hospital around midnight.

He was heavily sedated in the ICU, the doctor said, hooked up a ventilator, with tubes in his trachea. To try to improve lung function, he had been flipped over onto his stomach.
While the situation was dire, family members were not allowed inside the hospital. The risk, public health experts had determined, was too great.
“My heart just ached,” said Silliman-Patterson, who is 47. “I didn’t want him to be scared. I didn’t want him to be alone.”
In yet another way the coronavirus is inflicting pain, the pandemic has robbed patients facing life-threatening illnesses of a key weapon as they fight to recover: family and friends by their bedsides. As part of the effort to stanch the spread of the highly contagious virus, visits to hospitals have been severely restricted — for patients suffering from COVID-19, as well as those with heart disease and cancer and a host of other critical illnesses.
The very sick are facing hospital stays without the support of the people most important in their lives. And some are dying, with the only communication from loved ones coming in the form of phone calls and messages.

It’s a devastating situation for both patients and those close to them.
“How do you cope when you are not able to see your loved ones in their last days or hours of life?” said Dr. David Ferraro, vice chair of the Society of Critical Care Medicine’s Fundamental Disaster Management Committee. “It’s very tragic for families, and there is a lot of closure that may not be able to happen.”
Overwhelmed health care workers do what they can to offer comfort, but they acknowledge they are no substitutes for spouses, children and friends.
The visitation restrictions are forcing medical workers to be “as creative as possible,” said Dr. Tammie Quest, director of the Emory Palliative Care Center.
Many hospitals are using iPads to allow patients to have virtual visits with family members and are turning to video conferencing to provide family members updates.
Pam Redman, Piedmont Atlanta’s director of patient experience, said health care workers also are trying to fill the void by spending more time with patients. If patients are up for it, they are supplying them with puzzles and magazines. Small tokens from members of the community, such as the homemade ribbon-and-crystal-bead angels, remind patients that many are thinking about them.
Those gestures “have made the biggest difference,” Redman said.
Hospitals also work to connect patients with their priests, rabbis or other spiritual leaders. In some cases, chaplains are allowed to visit, wearing protective gear or standing outside the room. One of Wellstar’s chaplains recently reached out to the son of a patient to help facilitate a conversation, said Renee Owen, executive director of spiritual health for Wellstar. The son wanted to tell his critically ill dad he loved him. The chaplain was able to put a phone up to the father’s ear.

Waiting for updates
Silliman-Patterson, who lives only a couple miles away from the hospital, felt frozen in time. She tried to read or knit, but couldn’t. She found herself just waiting for updates on the man she fell in love with more than 25 years ago as a college student. Though they had divorced five years ago, the two managed to stay close friends as they co-parented their children: Thomas, who is 26; Alex, 24; Josh, 21; and SarahBeth, 15.

Two years ago, when Lindsey’s apartment burned down, he moved into Silliman-Patterson’s basement for six months until he found a new place.
A laid-back man who loved tai chi, playing guitar and exploring the Clyde Shepherd Nature Preserve, Lindsey developed a cough on March 17 or March 18. At first, a family doctor thought it might be caused by acid reflux. But Lindsey got progressively worse. After seeking medical treatment on April 2, he seemed to be improving. But his condition suddenly worsened. On April 4, he made the midnight trip to the emergency room.
One of his sons, Alex, followed him in another car. His father refused to accept a ride because he didn’t want to expose him to the virus.

As she hoped for him to get better, Silliman-Patterson kept the phone close. When she took a bath, she didn’t put her ears under water, afraid she might miss a call from a doctor or nurse. Still, every time the call came, her stomach turned, dreading bad news. She usually stepped outside to talk, sitting on a curb under the spring sunshine. After each phone call, she contacted her in-laws; her sons, oldest to youngest; then told her daughter in person.
One evening at about 11:45 p.m., a nurse called during her break. She put the phone up to Lindsey’s ear so that he could hear Silliman-Patterson’s voice. It was a kind gesture, greatly appreciated. An ICU doctor also gave Silliman-Patterson his email address so the family could write letters. The medical team promised to read each one.
Silliman-Patterson said the staff was compassionate as workers search for ways to improvise.
“The doctors and nurses kept telling me he is not alone. They told me he was like family to them,” she said. “They were incredibly kind, and I know it was incredibly difficult for them.”
Isolating patients is gut wrenching for both families and medical workers, said Nadine Kaslow, an Emory psychiatry and behavioral sciences professor who is leading an effort to provide mental health support to front-line health care workers and the public.
“I can’t even imagine not being able to hold my loved one,” said Kaslow, starting to tear up. “Nobody wants to die alone. It’s awful for the patient. It’s awful for the family. It’s traumatic for health care workers.

Looking for the light
On the evening of April 11, seven days after Lindsey was admitted to the hospital, Silliman-Patterson got a call around 9:30 p.m. and fell to the floor.
Thirteen minutes earlier, she was told, Lindsey had died. Her daughter rushed into her room and they held each other at the foot of bed and cried. Silliman-Patterson then called her sons and Lindsey’s parents.
She grieves for her children, who couldn’t see their father before he died.
“My kids were robbed of that. We are going to have a generation this happens to. This is a group trauma we are experiencing. And how we are going to come out of this, I don’t know.”
The day after Lindsey’s death, his family gathered in the car port, with wind chimes playing notes. The minister at Decatur Presbyterian Church led a prayer. A candle flame flickered, and the family said they felt Lindsey’s presence.
In a Facebook post, Silliman-Patterson talked about how Lindsey radiated in their children, their laughter and their love for each other. And, in another post just two days after Lindsey’s death, she encouraged everyone to look for light — in the darkness.
Sometimes the world is full of darkness and, if we aren't careful, we can allow evil to prevail. Look for the light, turn the other cheek. Live in peace. If we are to emerge from this, we need to join together and look for the goodness. Living with hate and animosity and spreading that does nobody any good. Be kind. Do something kind for someone today.


