Inside Savannah hospital, staff manages deluge of COVID patients

SAVANNAH — Walk through the COVID-19 wards of this city’s largest hospital and things seem eerily calm.
No doctors or nurses running or shouting under the fluorescent lights. No gurneys crowding the hallways or patients who are gasping for air overflowing into the lobby. Just the continual beep of the vital signs monitor hanging in front of the nurses’ station.
But make no mistake, the staff working the coronavirus floors of Memorial Health University Medical Center says. The scenes playing out behind the closed doors of each patient’s room are increasingly dire.
As the ultra-contagious delta variant continues to tear across the Southeast, the COVID-19 patients hospitalized here are sicker and stay longer than those earlier in the pandemic. They’re younger and require more care, more resources, more ventilators. And there have been way more of them than at any other point over the past 18 months, despite the widespread availability of vaccines.
Memorial Health cared for a record-high 178 COVID-19 patients at the end of August, according to the hospital. That’s more than twice as many as it did during previous pandemic peaks, said Dr. Stephen Thacker, the hospital’s associate chief medical officer. The week the Atlanta Journal-Constitution visited Savannah in early September, Georgia reported the country’s fourth-highest number of COVID-19 hospital admissions.

By many accounts, Memorial Health has fared better than other hospitals in the region, though. The 645-bed facility, which serves 35 counties across Southeast Georgia, was built to absorb shocks to the system, with the space and equipment to care for the patients requiring advanced medical attention that smaller and more rural hospitals can’t provide.
Still, the scope and severity of the delta wave are straining even the state’s largest and most well-resourced hospitals. Like other major providers inside and outside of metro Atlanta, Memorial Health has at times turned down patients from elsewhere to keep up with surging coronavirus caseloads, in addition to the heart attacks, gunshot wounds and other everyday emergencies that have continued in the wake of the pandemic.

The week of Sept. 2, patients occupied more than 95% of the hospital’s inpatient beds and all 184 inpatient ICU beds. In Chatham County that week, COVID-19 patients filled 45% of staffed adult ICU beds.
Since then, new COVID-19 hospitalizations have declined significantly in Chatham, yet upward of 95% of inpatient and ICU beds are still occupied, according to the federal Department of Health and Human Services. On Wednesday, Memorial Health said it was treating just 85 COVID-19 patients, 30 of whom were in the ICU, and an additional 42 patients who previously had the virus but were still in the hospital.
The up-and-down has tested exhausted frontline workers and administrators, many of whom are worried about what’s to come this fall, with inoculation rates remaining stubbornly low, schools meeting in-person and colder weather moving many social gatherings inside.
“It’s not something that I would ever wish on my worst enemy,” said Amber Dixon, a respiratory therapist who’s been working in the COVID-19 ICU since spring 2020. “Our days are very long and, to put it bluntly, we see a lot of death.”

Overhauling operations
The third and fourth floors of Memorial Health’s Heart and Vascular Institute weren’t designed to house COVID-19 patients.
Both were renovated right before the pandemic to accommodate cardiac cases and a medical ICU. But within weeks of hospital executives cutting the ribbon in January 2020, they were converted into COVID-19 wards — one reserved for more seriously ill patients who need help breathing and the other for patients with less severe symptoms.
Situated on a sprawling campus dotted with palms and magnolia trees on the eastern edge of the city, Memorial Health — like every hospital in the country — has been forced to overhaul its operations to respond to the pandemic.
In addition to increasing the number of beds dedicated to coronavirus patients, hospital officials have shifted staff from other departments to aid the ICU during surges and recently opted to halt elective surgeries again to free up additional workers.
The hospital once struggled financially before being acquired by the for-profit chain HCA Healthcare in 2017. Thacker said HCA’s network has helped Memorial Health secure personal protective gear and in-demand equipment like ventilators.

“Thankfully we’ve not been put in a position that has limited our ability to meet the immediate emergent needs of our local community,” said Thacker, who’s also a pediatric infectious disease specialist.
However, finding and retaining enough staff to operate that equipment and care for those patients has been difficult. Hospitals are essentially poaching nurses from one another amid a nationwide nursing shortage. Memorial Health wouldn’t discuss the number of empty positions on staff but said it’s brought on visiting nurses, who tend to be pricey but can fill critical gaps during upticks.
Respiratory therapists like Dixon are in particularly high demand. Memorial Health uses a software program to estimate how much staff is needed to care for the number of patients who require ventilators or breathing treatments. That software recently showed that based on current levels, the hospital ideally needs nearly twice as many respiratory therapists as it currently has on staff, said Dixon.
“It doesn’t matter how many machines you have if you don’t have the staff to run the machines,” she said. “We’re having to cover a larger area because we have so many critically ill patients.”
More of those patients require drugs to keep their hearts beating or elevate their blood pressure, to pump their organs with oxygen and fluids to help them stay alive. Particularly disheartening is that some seem to be improving and in relatively stable condition, only for their condition to take a sharp turn within minutes.
“It’s really hard to see patients come in who initially are walking and talking and are requiring small amounts of (care), and then you see them very quickly progress into respiratory distress,” Dixon said.
Unlike some hospitals in New York early in the pandemic — or in north Georgia more recently — Memorial Health hasn’t been forced to treat patients in hallways, tents or ambulances in the parking lot to keep up with new admissions.
“It doesn't matter how many machines you have if you don't have the staff to run the machines."
But there have been moments when beds are full. At those times, sick patients who have been cleared for admission must stay in the hospital’s emergency room or, on occasion, its post-anesthesia care unit to wait for others to be discharged — which can sometimes take minutes or hours. Memorial Health declined to say how many patients had backed up in the facility recently waiting for beds but stressed that “our team members do an exceptional job of caring for our patients wherever they are.”
The day before the AJC’s visit, multiple sections of the hospital were on diversion, meaning they were so overburdened that they were urging ambulances to ferry sick patients to other hospitals. Some smaller hospitals in the region, including Hazlehurst’s Jeff Davis Hospital, said they’ve recently had patient transfer requests turned down by Memorial Health.

The hospital wouldn’t comment directly about Hazlehurst, but a spokeswoman said “even though our goal is to offer our exceptional care to patients from other hospitals, we aren’t always able to take a transfer. This is what happened during the most recent COVID-19 peak as we cared for a record number of cases in our immediate area.”
Thacker said Memorial Health was “not sending people away.” At the same time, as the region’s only state-designated Level I trauma center, the hospital must be ready to take the most serious emergencies and injuries.
“We need to make sure we can continue to care for the patients we have currently admitted safely, but also be prepared for what we know is going to come in our front doors because we’re a very busy ER,” Thacker said.
‘Heavy thing to carry’
The crushing pace has weighed heavy on the staff, some of whom have worked the ICU floor since March 2020.
One of those frontline workers is Kamika Shivers, a registered ICU nurse who was charged with caring for Savannah’s first-ever coronavirus patient last year. She compared the waves of the pandemic to hurricane seasons.
“You have some seasons that are just rain, and then you have Irma that came in and just wiped us out,” said Shivers, who grew up in the area and has been in the profession for roughly 14 years.
“This one,” Shivers said, “is just vicious.”
In some ways, however, caring for COVID-19 patients is easier than it was earlier in the pandemic, she said. The medical profession knows much more about the virus, how it spreads and the best way to care for those stricken. Gone are the space suits of last year. Nurses now don blue plastic gowns, N-95 masks, gloves and a face shield while caring for COVID patients, who are placed in negative pressure rooms that prevent infectious air particles from flowing into the hallway or other rooms.
Delta’s challenge is that it’s making people much sicker for longer. Nurses used to spend 20 minutes at a time with a patient, who’d generally stay in their care for three to five days. Now patients need closer to 30 or 45 minutes, Shivers said, and some stay for weeks.
“It’s sad to say that we’ve gotten accustomed to doing this,” Shivers said. “We’re just having to increase our level of care … as the acuity of the patient changes.”

All of that takes an emotional toll on workers.
Patients are increasingly in their 20s and 30s, some the parents of small children. Others are in such bad shape when they’re admitted that they can’t even communicate with the people who will try to save their lives — doctors and nurses are often left to glean whatever medical history they can from relatives on FaceTime. The ban on visitors only adds to the burden.
“Not only do we kind of take on the role of the health care provider, but we are also taking on the role of being a support system for them because they have no one else,” Dixon, the respiratory therapist, said in an interview in the hospital waiting room, a space that would normally be buzzing with families and friends of patients but instead sat empty on a recent Thursday morning. “It’s a heavy thing to carry.”
Staff burnout is a problem high on the minds of hospital administrators like Thacker.
Officials have tried to make themselves more available to their employees. Nurses and doctors have closed ranks. Local restaurants and community members have donated meals to boost morale, but many frontline workers admit they’ve had a hard time processing the onslaught.
“There is always somebody that needs attention. And so I think sometimes it is easier to just stay busy and keep looking for the next person to try to help or the next family to try to talk to than it is to actually reflect on the impact that it may have on me or my family,” said Dr. John Watson, an ICU physician who had moved to Savannah three weeks earlier.
“At some point, I hope we are all way behind this and I’ll have time to think about it, but we’re not there yet unfortunately,” he added.

A critical relief valve, according to Thacker, was Gov. Brian Kemp’s recent redeployment of National Guard and Georgia Emergency Management and Homeland Security Agency members to help overburdened hospitals. Many of the 17 to 20 guardsmen assigned to Memorial Health are being used for non-medical and clerical duties like directing traffic, answering phone calls and helping sedated COVID patients breathe by flipping them onto their stomachs. Fourteen GEMA nurses and four respiratory therapists have also helped give medical staff some time off.
“That type of support goes a long way to show our health care teams that the state recognizes that this is a tough time and is trying to provide resources where they can,” Thacker said.
‘What we do’
But the state’s help isn’t helping change the minds of the vaccine hesitant or resistant who make up the vast majority of coronavirus cases here. Forty percent of Chatham County’s population is fully inoculated, less than the statewide rate of 42.8%.
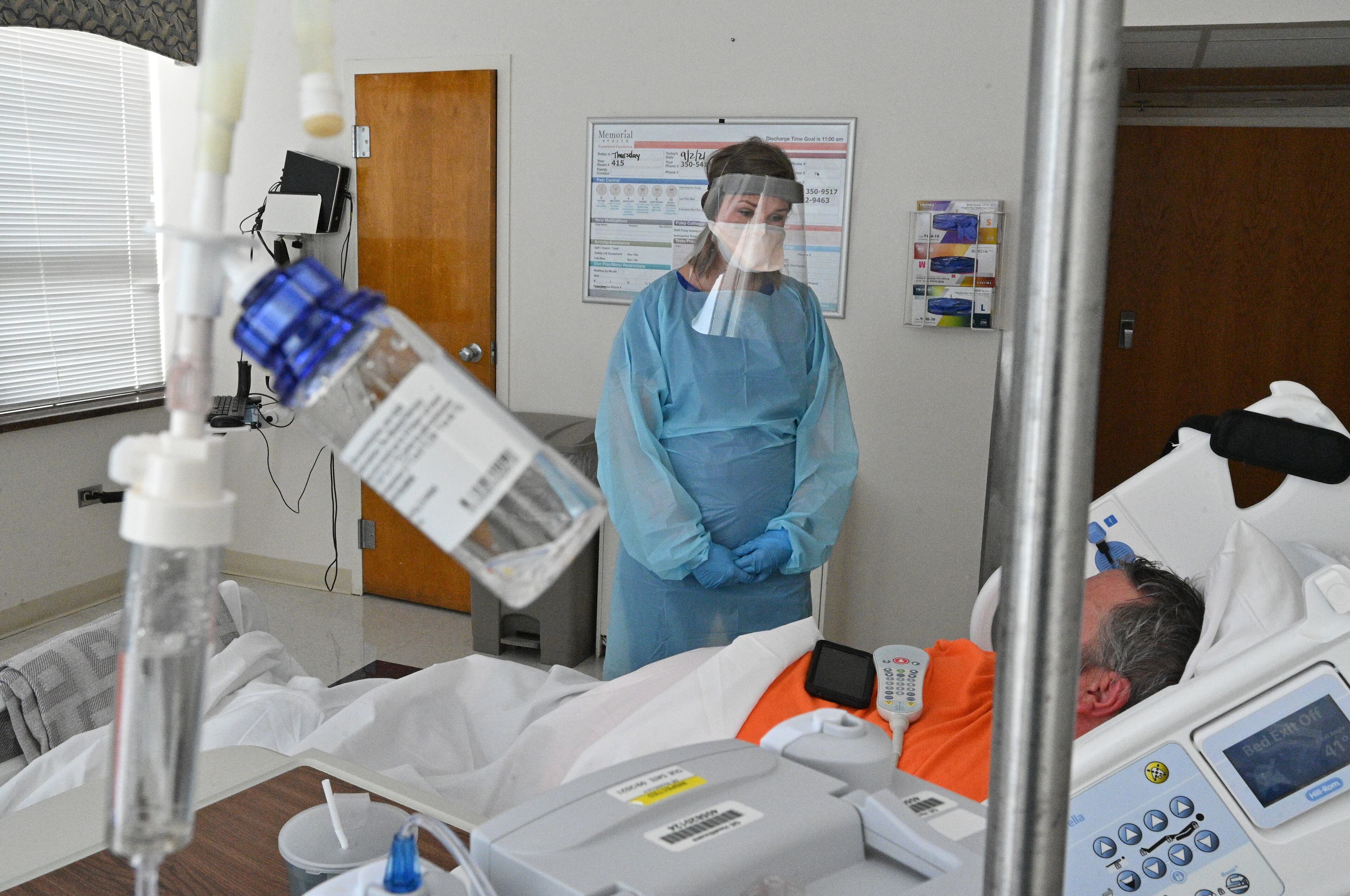
In a sun-drenched isolation room on the fourth floor of Memorial Health’s main building lay a 46-year-old Savannah man with streaks of gray running through a scraggly brown beard.
The man, who works for a drywall company and requested anonymity to discuss his health, had been admitted two days earlier after running a fever, feeling lethargic and nauseated a few hours after receiving an antibody infusion to treat COVID-19.
He had just received the good news that he was being discharged the next day. But despite his obesity, which increases the risk of severe COVID-19 illness, and feeling like a “human pin cushion” while being pricked with needles at the hospital, the man said he was still unsure about whether to get inoculated.
“To me this COVID vaccine came together really quickly,” he said. “I’m not saying I’m against it, I just want to see more data before I take that leap.”
In the meantime, the man said he hopes he’s built up enough antibodies to help him avoid another COVID-19 infection. But other than getting his blood pressure under control he said he doesn’t plan to change the way he lives his life to prevent another infection.
“I don’t even take the flu shot,” he said.
With delta, hospitals can one week see a flood of patients and the next have half-empty ICUs. The rollercoaster leaves some medical workers frustrated. They’ve worked long hours and made sacrifices in their personal lives — one nurse said she’s refrained entirely from visiting her sick father — only to see caseloads yo-yo.
At one point earlier this summer, Shivers’ ICU ward had only one COVID-19 patient.
“We saw the light and could almost put our finger on it, almost,” she said. “Then the floodgates just opened up.”
In Georgia, COVID-19 hospitalizations reached their peak just before Labor Day and had declined some 10% by Sept. 13. But deaths are still sharply inclining: they doubled in August and are on track to double again in September.
Despite that, all of the frontline workers interviewed said they still see their work as their calling.
“I go home and vent my frustrations at the end of the day, but I’ll come back to work and do the same thing over and over again because this is the job I chose and this is the profession I love,” said Shivers. “It is frustrating and it’s tiresome but it’s what we do.”
But staff is still bracing for what could be a difficult next few months, especially at Memorial Health’s Dwaine & Cynthia Willett Children’s Hospital. Dr. Michael Bossak, a pediatrician there, is concerned that seasonal flu could stretch a workforce already overloaded with a deluge of respiratory illnesses and a growing number of COVID-19 cases among children.
“It’s one of those things where we look at the numbers and think that we have enough to take care of everybody, but we’ll never know until we get there,” Bossak said. “COVID is this unknown.”


