The fragile state of Georgia health care

Veronica G. Brown needs a hip replacement. But, like 1.5 million other Georgians, she doesn’t have health insurance.
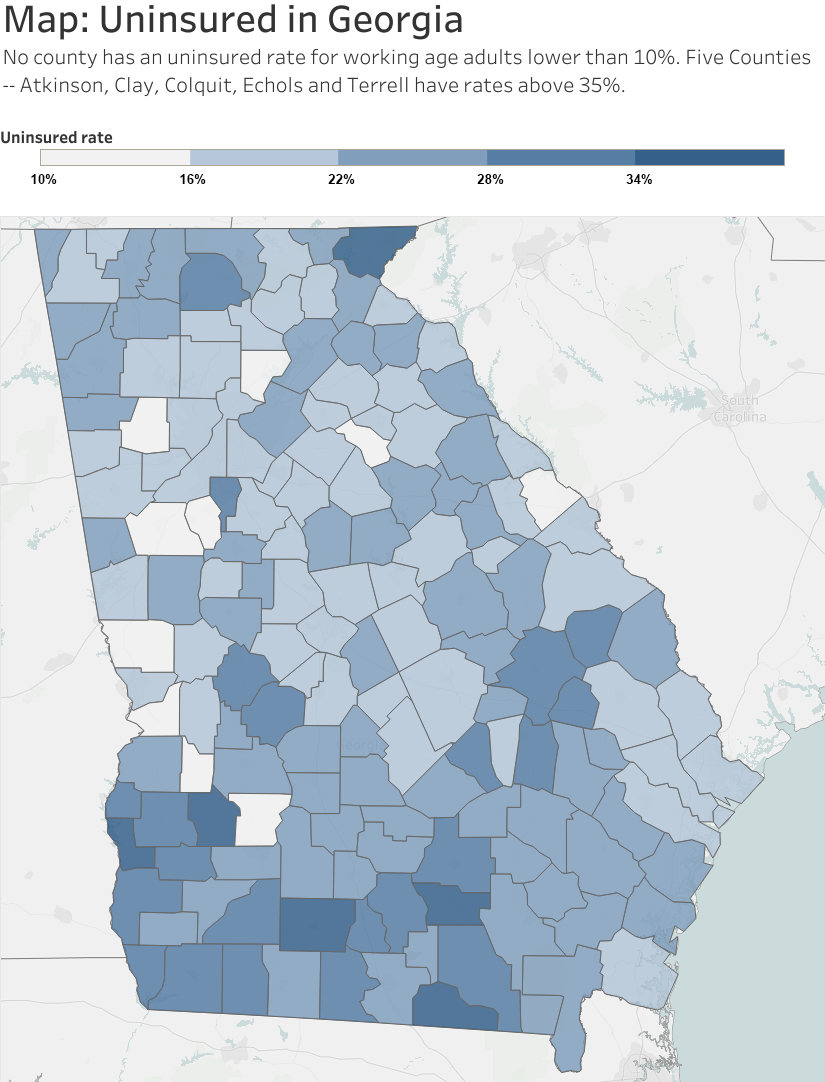
That’s a big number. It’s about 1 out of every 7 Georgians. And it has the governor’s attention.
Enabled by a new law granting him a budget and power to draw up new health care proposals for the state, Gov. Brian Kemp hired the consulting firm Deloitte to report back to him on the landscape of Georgia health care. The goal of the report is to help him chart the new path. He recently got Deloitte’s findings.
They're challenging. The Atlanta Journal-Constitution is laying out some of the highlights here.
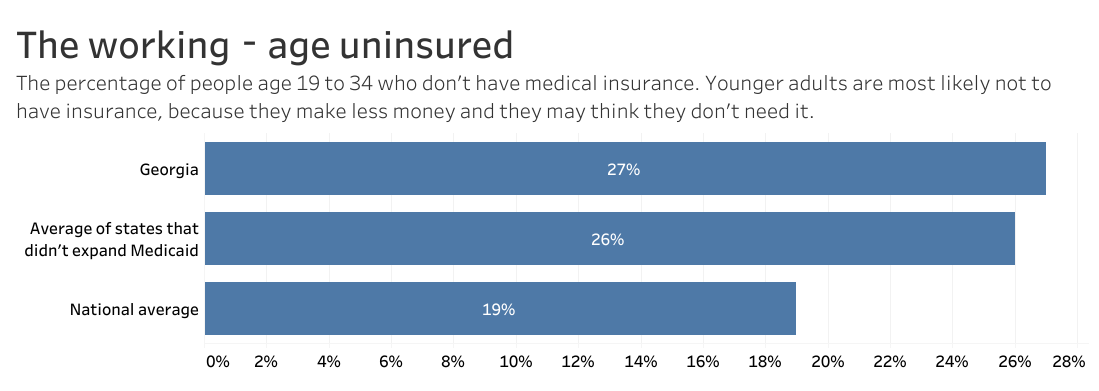
Georgia has worse access to health care than most states, such as available doctors and mental health care providers. In one recent year, 17% of Georgians said they needed to see a doctor in the past 12 months but couldn’t because of cost.
>> Related: By the numbers: Health care in Georgia
And it shows in health outcomes. Georgia, the home of nationally known hospitals and other top health programs, ranks in the bottom one-third of states for the health outcomes of its residents, such as premature deaths, infant mortality or diabetes.
Kemp has not said much about what plan he’s leaning toward. He will not propose to expand Medicaid to all of Georgia’s poor, a position his aides staked out on the campaign trail and that his office as governor helped write into law. He may decide to start small with pilot programs.
For Brown, the numbers are personal.
She’s nine months sober and residing in a transitional living facility after decades of addiction and said she’s “elated” at her life. But it’s time to find a job, and the hip is a problem.
She has no cartilage left to cushion the joint and must alternate between standing and sitting.
“I’m really in a Catch-22 position and it saddens my heart,” Brown said.
Georgia didn’t expand Medicaid under the Affordable Care Act to cover all its poor adults. So at 53, Brown doesn’t qualify. She’s not old enough for Medicare yet, which starts at 65. She has no income, so she doesn’t qualify for an insurance plan under the ACA.
Mercy Care, a charity in downtown Atlanta, gave her pills for inflammation that didn’t help, but it can’t do the surgery.
Large numbers of uninsured means people who don’t get care until it’s an emergency, or ever. It means people who get care in emergency rooms, leaving hospitals and caregivers with unpaid bills.
What was in the Deloitte report was already known to policy wonks, said Bill Custer, a health analyst at Georgia State University. But knowing it could lead to action by the governor gives it new meaning.
“Clearly it’s not a lost cause,” Custer said.
Sources for these graphics: Georgia Department of Community Health report by Deloitte Consulting, and America’s Health Rankings. The DCH/Deloitte sources include the U.S. census, SHADAC, Kaiser Family Foundation, America’s Health Rankings and others.