U.S. vaccinations ramp up as second COVID-19 shot nears
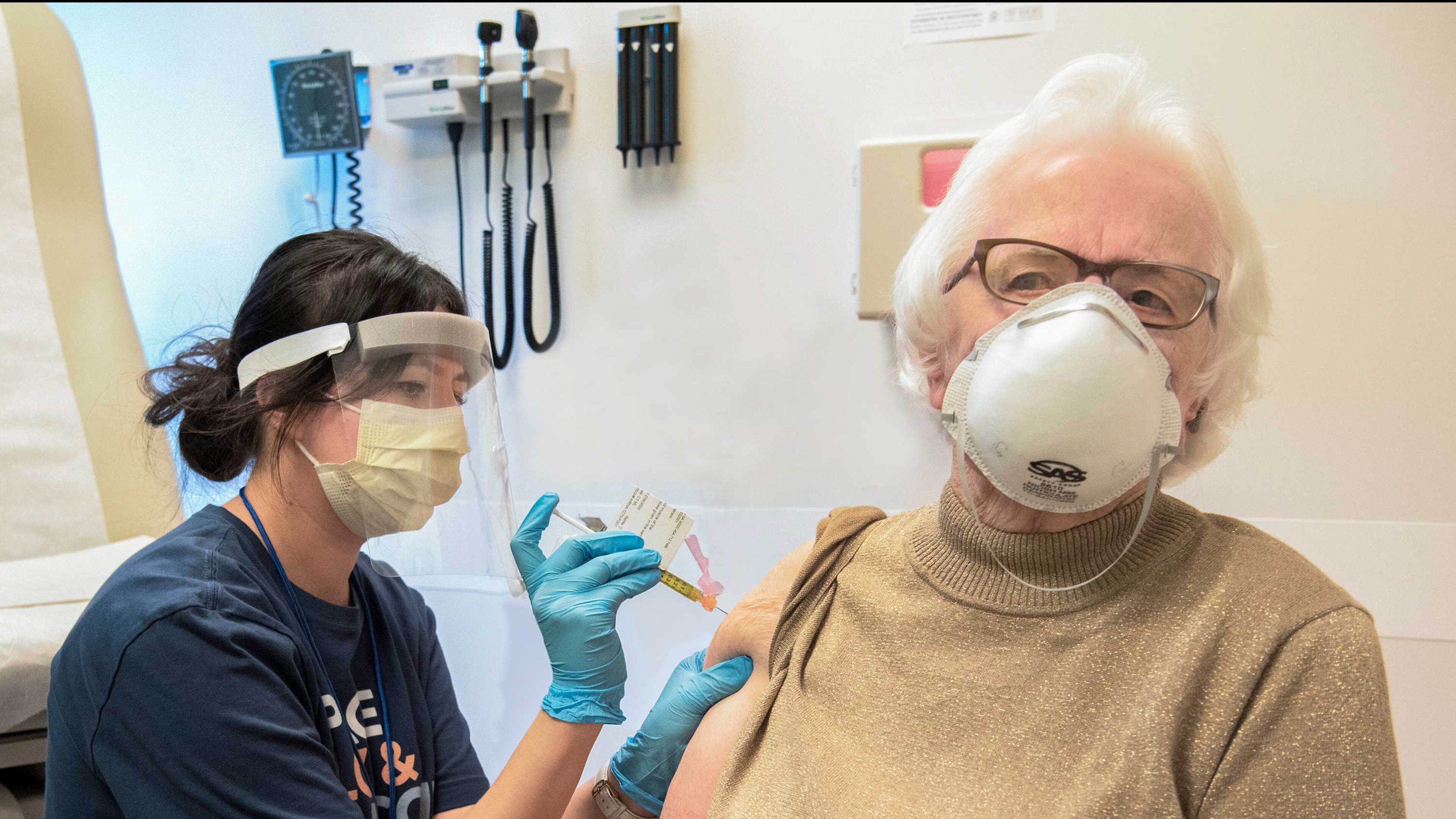
WASHINGTON — Hundreds more U.S. hospitals geared up to vaccinate their workers Tuesday as federal regulators issued a positive review of a second COVID-19 vaccine needed to boost the nation’s largest vaccination campaign.
The Food and Drug Administration said its preliminary analysis confirmed the effectiveness and safety of the vaccine developed by Moderna and the National Institutes of Health, bringing it to the cusp of U.S. authorization.
A panel of outside experts will offer their recommendation Thursday, with a final FDA decision expected soon thereafter.
The positive news comes as hospitals ramped up vaccinations with the shot developed by Pfizer and BioNTech, which the FDA cleared last week.
Packed in dry ice to stay at ultra-frozen temperatures, shipments of Pfizer’s COVID-19 vaccine will arrive at 400 additional hospitals and other distribution sites, one day after the nation’s death toll surpassed a staggering 300,000. The first 3 million shots are being strictly rationed to frontline health workers and elder-care patients, with hundreds of millions more shots needed over the coming months to protect most Americans.
A second vaccine can’t come soon enough as the country’s daily death count continues to top 2,400 amid more than 210,000 new daily cases, based on weekly averages of data compiled by Johns Hopkins University. The devastating toll is expected to only grow in coming weeks, fueled by holiday travel, family gatherings and lax adherence to basic public health measures.
The first vaccine deliveries have provided a measure of encouragement to exhausted doctors, nurses and hospital staffers around the country.
Johnnie Peoples, a 43-year-old survival flight nurse, was excited and a little nervous Monday afternoon as he unzipped his flight suit and stuck out his left arm to become the first person to receive the vaccine at the University of Michigan Medical Center in Ann Arbor.
“Just to be a part of it is a good feeling,’' he said.
Since March, he’s transported critically ill COVID-19 patients by jet from smaller hospitals around the state to the university medical center. It’s up-close-and-personal work that requires him to adjust ventilator settings and administer infusions to keep blood pressure from plummeting.
In Florida, government officials expect to have 100,000 doses of the vaccine by Tuesday at five hospitals across the state.
“This is 20,000 doses of hope,” said John Couris, president and chief executive officer, Tampa General Hospital, after the delivery of 3,900 vaccine vials Monday. Each vial has five doses.
Because the vaccine requires two rounds, the people getting injections now will need a second shot in about three weeks.
Moderna’s vaccine is the same type as Pfizer’s, made with the same technology. And in scrutinizing early results of a 30,000-person study, the FDA found it also worked just about the same.
The Moderna vaccine was more than 94% effective overall at preventing COVID-19 illness and 86% effective in people 65 and older. The FDA uncovered no major safety issues.
Recipients tend to experience temporary flu-like side effects that can include fever, fatigue and aches, especially after the second dose as the vaccine revs up their immune system.
Even such a large study can’t detect very rare problems. But the FDA looked carefully for signs of allergic reactions after Britain last week reported some possible reactions among people with a history of severe allergies.
The FDA found no serious allergic reactions in the Moderna study. About 1.5% of vaccine recipients and 1.1% who got dummy shots reported possible smaller, “hypersensitivity” reactions.
Moderna’s and Pfizer-BioNTech’s shots are so-called mRNA vaccines. They aren’t made with the coronavirus itself, meaning there’s no chance anyone could catch it from the shots. Instead, the vaccine contains a piece of genetic code that trains the immune system to recognize the spiked protein on the surface of the virus.

