Now 4 for 4, Grady’s Ebola EMTs on a roll
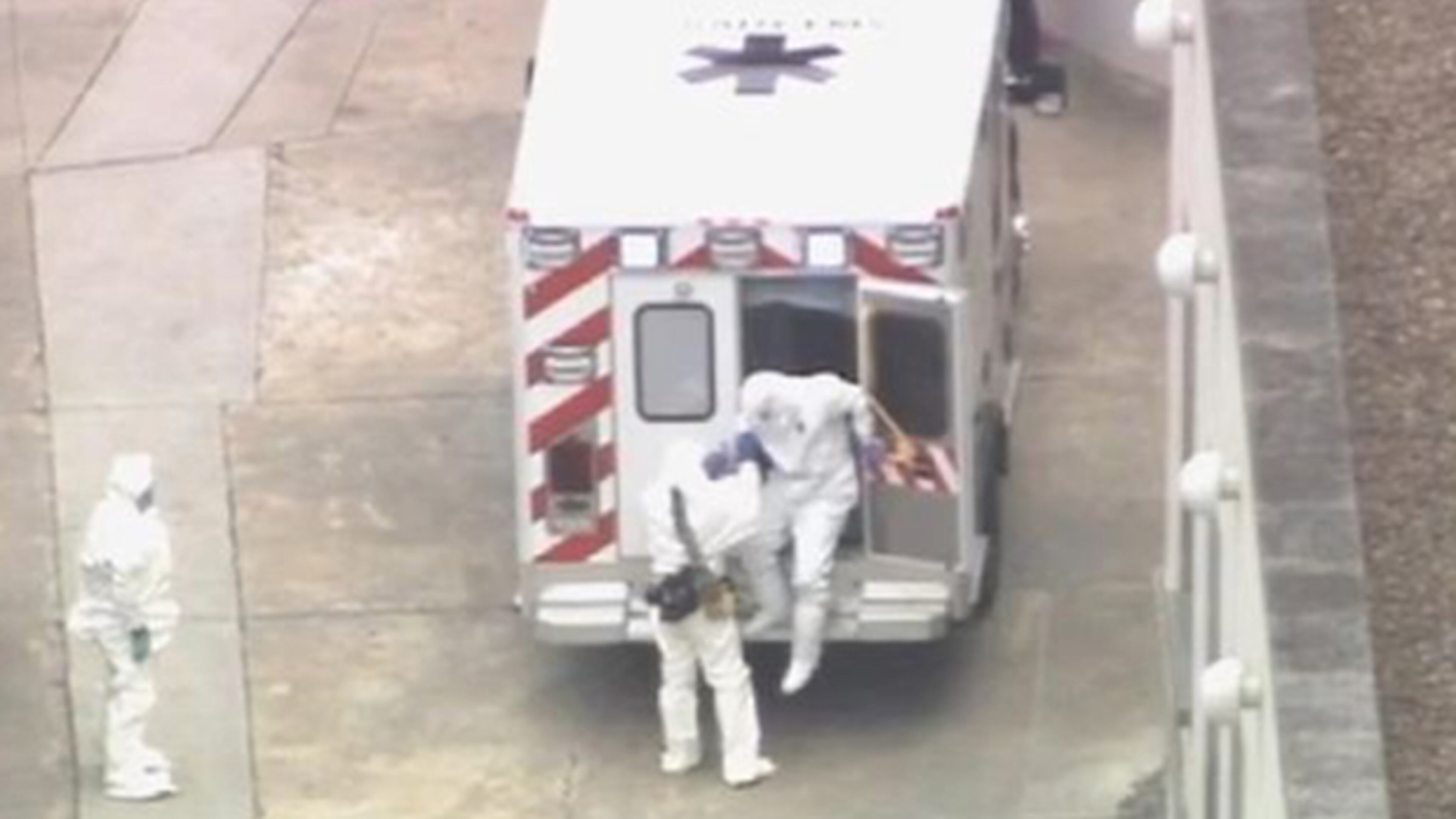
A critical leg of an Ebola patient’s journey to the isolation unit at Emory University Hospital starts at the edge of Cabbagetown.
There, inside a nondescript building off Memorial Drive, Black Sabbath’s “Heaven and Hell” blasts over speakers as the Special Operations transport team of Grady Memorial Hospital prepares: Gail Stallings, John Arevalo, Wade Miles, Aaron Jamison. The music centers them as much for the task ahead as a prayer.
The team of EMTs is four for four: Dr. Kent Brantly; missionary Nancy Writebol; an anonymous World Health Organization doctor; and Texas nurse Amber Vinson. All four were delivered to Emory without incident and, so far, without any teammate contracting the lethal virus.
They ought to be good at this. They’ve been practicing for more than 10 years.
***
Arevalo is talking about their first Ebola call: taking Brantly from Dobbins Air Reserve Base in Marietta to Emory University Hospital. Arevalo, 34, says he felt no fear when he walked Brantly, also swathed in protective gear, into Emory’s isolation unit under the glare of news cameras.
“It was an honor to be there when almost the whole nation was against them,” Arevalo said. “Everybody was like, ‘No, no, don’t bring them here.’ Then for us to be the ones who were like, ‘You know what? We’re going to take care of our own. We’re going to bring you home, we’re gonna be there for you,’ that was an honor.”
Stallings adds that, despite the muffling effects of the protective suits, among the first words the early patients heard from the Grady team were “Welcome home.”
Team members may be unafraid, but they still have to deal with the perceptions of others.
Miles and Arevalo are both married to nurses, who they say understand. But Miles, 41, has neighbors who are now a little standoffish because they know his role in this national saga, he said.
Arevalo’s stepdaughter was having a manicure recently when news footage of the team ran on a television in the salon. Proudly, she said, ‘That’s my dad.” The client sitting next to her promptly asked to be moved across the salon.
“It doesn’t have to be scary,” said Stallings, 42. “Fear tends to be a snowball that runs away with people and gets very hard to stop. But all you need is a little bit of knowledge to slow it down. There are so many other things that people should be concerned about, like the flu. But we’re focused on this because it’s an unknown.”
***
In a charged environment where at least one American hospital has stumbled horribly while caring for an Ebola patient, and where others are scrambling to prepare for the potential arrival of their first, the Grady special ops people are proven veterans.
Last week, in the office of their Cabbagetown bunker, the entire team sat down with The Atlanta Journal-Constitution to talk about their role in the treatment of the disease in the U.S.
Laid back, they ribbed each other, finished each other’s sentences and shared easy laughter. They weren’t so much cocky as assured. There was respect for each other, but, most important, respect for the deadly potential of the virus.
“It all goes back to training, knowledge and trust,” said Stallings.
The unit’s origin is rooted in police operations. Though it is a volunteer group, paramedics have to go through a rigorous application and screening process to join. Jamison, a 23-year Army veteran, and Miles helped start the special ops division about 12 years ago to assist the Atlanta Police Department’s SWAT team. If an officer was injured in a raid, the special ops team was the first responder.
Around the same time the Grady team was founded, Emory University was building its biocontainment unit in conjunction with the CDC and needed a specialized team to transport patients. The biocontainment chambers were designed specifically to treat CDC workers exposed to lethal pathogens on the job, Miles said.
Over the years, Wade, Jamison, Stallings and Arevalo have literally burned through 300 hazmat suits used on assignments and training sessions, Jamison said. They also had their regular duties as paramedics.
“Everybody knew it was just a matter of time before we got activated” on a major infectious disease case, Arevalo said.
In the meantime, they waited, studied and trained for dealing with Level 4 viruses: diseases with no approved treatment drugs or vaccines. Along with Lassa fever and Marburg virus, Ebola was just one of the many they had to be ready for.
Jamison is the wiseguy of the group, 52 years old with a thin beard and skin weathered from years spent outdoors. His combat experience has shaped the way he assesses threat. The only way to prepare for any type of enemy, biological or otherwise, is to train, he said. The team has done at least quarterly drills for the past decade.
“There’s no short cuts,” Stallings, 42, said. “Short cuts are where mistakes happen. You start making short cuts and then that short cut becomes a habit, and then, when you have something big, something goes wrong.”
***
All four are barred from talking about what goes on in the ambulance, including conversations they had with patients. Apart from ethical reasons, there is a practical one: it’s difficult to talk and hear once they are in full protective gear. It’s one of the reasons that donning the suits is one of the last things they do.
“Think about putting yourself in two Ziplock bags,” Jamison said.
“That don’t breathe,” said Arevalo.
“Then throw you in the sunshine and it starts to condensate,” Jamison said.
Even though the suits draw air in through a filtering system, they become “little, mini personal saunas” within 20 minutes, Stallings said. The team works in them for up to eight hours.
Because the suits also create tunnel vision, body language becomes as important a component of patient care as anything.
***
The calls always begin the same way, with “some crazy heavy metal,” Arevalo said, usually of Jamison’s choosing. When Jamison pulls out “the book,” the process of preparing for an Ebola patient really begins.
“The book” is the sum of the team’s learning on how to handle Ebola and other deadly infectious diseases. It’s a checklist they have followed, letter by letter, each time they’ve transported an Ebola patient. The team members switch off, playing different roles in the transport process. But they never deviate from the script for each specific role. (Nor have they changed the kind of music they listen to as they get ready).
For Brantly’s pickup, Arevalo and Stallings got the vehicles ready. Jamison checked the filters and batteries in the respirators to make sure none was expired and gathered other supplies. Miles, the team’s director, was in contact with the State Department, the FBI, Emory and Grady’s medical director. Stallings drove the main ambulance and Arevalo was in the back with Brantly. For Writebol, Jamison took the wheel, with Arevalo and Stallings in back because Writebol was too weak to walk.
Since their first case the team has been flooded with emails from health care workers from as far away as New Zealand seeking advice on how to prepare for an Ebola patient. At the request of the CDC, Miles was even flown to Dallas to supervise the ambulance clean-up there after Amber Vinson’s transport.
“I was not the clipboard man,” Miles said, referring to a man on the tarmac wearing only street clothes who was working with the team loading Vinson onto the plane.
Here, when they clean an ambulance, they do not use the buddy system. In fact, they don’t use the buddy system in any stage of the prep or clean up. They use an “arena” system, with at least two sets of eyes watching the person performing a task, whether cleaning the ambulance or taking off gear. One person calls out directions, the rest watch, making sure commands are followed.
Afterward, they sit down, drink endless bottles of water and talk about what went right, what went wrong and what can be improved upon. While they are hopeful they won’t have to handle another U.S. Ebola patient, they say they are ready, nonetheless.
“Just to know that we played a small part in getting these patients the care that they needed and then they leave and go home to their families, that’s a good feeling,” Miles said.

